Not Enough Doors, Too Many Gaps: Why Education Isn’t Producing the Healthcare Workforce We Need
By Van Ton-Quinlivan
Think about the number of disconnected systems a learner must navigate to move from education into employment, especially in healthcare. What should be a pathway often feels more like a maze. A single workforce program can involve multiple handoffs: recruitment and screening, coursework through a community college or alternative provider, clinical placement with an employer, state exam preparation through yet another entity, and finally job placement and coaching. Each step may work well on its own, but together they rarely function as a coherent system.

At Futuro Health, we set out to simplify this learner journey, especially for adults from underserved communities. What began as a collaboration among healthcare education institutions has evolved into a growing ecosystem, one that now spans nine states and has expanded to include 43 vetted higher education partners sharing standardized practices.
That growth has required us to rethink what collaboration actually looks like in practice. As we entered rural geographies, such as parts of Connecticut, we partnered with smaller colleges that offered strong programs but have limited capacity to track workforce outcomes. In many cases, a single staff member was responsible for everything from accounting to following up on job placement.
Rather than turning these institutions away, we chose to invest in their growth. We are building additional shared tools and standards, helping our education partners strengthen their recordkeeping, improve accountability, and better demonstrate outcomes as well as improve interventions — when we together monitor the progress of Futuro Health Scholars on a weekly basis.
We have learned from our partners and iterated on what effective collaboration can be. The field-level infrastructure we are building continues to reduce friction for both learners and employers. Success is no longer dependent on a heroic coach or a single high-performing institution; it is embedded in a system designed for adults to earn a healthcare credential that jump starts their first or next career.
At a time when higher education is being challenged by a loss of public trust in institutions, survival may depend on heightened collaboration. The institutions that learn to work together—sharing data, aligning pathways, and co-investing in outcomes—will be the ones that endure.
This challenge is not unique to healthcare. Over the past two decades, the connection between education and employment has weakened across the economy. College graduates are taking longer to secure their first job, and the advantage of a degree, while still real, is no longer as immediate or assured. The issue is not simply access to education; it is the system’s ability to convert learning into work.
For healthcare, and increasingly across sectors, the imperative is clear: strengthen education providers so they can reliably deliver talent outcomes. That means building the shared infrastructure, data transparency, and collaborative capacity that turn programs into pathways and credentials into careers.
Without that shift, we will continue to create more doors but leave too many learners standing in the gaps.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader and formerly served as Executive Vice Chancellor of the California Community Colleges.
Does Place Still Matter? Rebundling Higher Education for an Unbundled World
By Van Ton-Quinlivan
In preparing for a recent lunchtime panel with the American Council on Education and its 800+ conference attendees—titled “Unbundled. Accelerated. Aligned.”—I found myself returning to a deceptively simple question: What is the value of “place” today, when learning can happen anywhere?

On my panel were executives from Coursera and edX, platforms that collectively reach hundreds of millions of learners worldwide. We were preparing for a provocative discussion—one that would challenge long-held assumptions about the primacy of the physical campus.
For more than a century, colleges and universities have earned public trust by bundling multiple functions into a single, cohesive experience: content, instruction, assessment, credentials, learner support, and community. This campus-based model didn’t just deliver education—it expanded access, fueled innovation, and helped build the American middle class. “Place” mattered because it concentrated opportunity. It signaled quality. It created belonging.
But that bundle is no longer fixed.
With the rise of online platforms, alternative credential providers, and employer-led training, learners now assemble their own pathways from a growing marketplace of options. AI will only accelerate this shift—lowering the cost of content, personalizing instruction, and reshaping assessment in ways we are only beginning to understand. The result is not just more choice, but more fragmentation. The bundle has been broken apart.
And yet, higher education’s role is not diminished—it is being redefined. The central question is no longer whether institutions will unbundle, but how they will rebundle in ways that are meaningful, differentiated, and aligned with today’s learners.
Rebundling higher education for today requires clarity of purpose.
As colleges and universities look to recruit beyond a shrinking pool of traditional high school graduates, they must decide which elements of the bundle are essential—and which can be partnered, outsourced, or reimagined.
Relevance becomes the first test.
What does it mean for learning to translate into economic mobility? Learners are increasingly pragmatic. They are asking: Will this program lead to a job? Will it help me advance? Institutions that can clearly connect learning to labor market outcomes—without reducing education to mere job training—will stand apart.
Human well-being is the second anchor.
If AI and automation reshape work, then distinctly human capabilities—communication, empathy, ethical judgment, resilience—grow in importance. This is where higher education has always had a quiet advantage. The question is whether institutions will lean into it more intentionally. Supporting the “whole learner” is not ancillary; it is central to long-term success in both life and work.
And then there is a third, often underappreciated function: the transfer of values.
As Joshua Travis Brown of the Johns Hopkins University School of Education shared with me on his recent appearance my on WorkforceRx podcast, colleges are not just sites of knowledge transmission—they are sites of values formation. Whether through athletics, service, religious life, or civic engagement, institutions pass along norms, identities, and a sense of shared purpose. In a distributed, digital-first world, this function becomes harder to replicate—and arguably more important.
Which brings us back to “place.”
If content can be accessed anywhere, then the value of place shifts from delivery to experience. Place becomes less about where you sit in a classroom and more about where you are known, challenged, and transformed. It is where relationships form—between peers, mentors, and networks that endure well beyond graduation. It is where learners test ideas, encounter difference, and develop a sense of self.
The future, then, is not a binary choice between physical campuses and digital platforms. It is a more intentional integration of both. The institutions that thrive will be those that stop trying to preserve the old bundle intact—and instead design new ones: modular, flexible, and deeply aligned to learner goals, while still preserving what only they can uniquely provide.
In a world of abundant access, place still matters.
But only if it stands for something unmistakably valuable
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader and formerly served as Executive Vice Chancellor of the California Community Colleges.
Rebuilding Trust in Higher Education
By Van Ton-Quinlivan
Recently, I attended the Ditchley–Lumina Summit, Redesigning Higher Education for the 21st Century, where an urgent question framed the conversation: how does the United States move from roughly 55 percent of adults holding a degree or credential of value to 75 percent
The Ditchley–Lumina Summit convened leaders from across the learning and workforce ecosystem — including Futuro Health, the Gates Foundation, Strada Education Foundation, ECMC Foundation, the American Council on Education, academics, think tanks, and student leaders — all committed to reimagining the #FutureOfLearning.

In the room were long-standing leaders of higher education — individuals who have devoted decades to strengthening our institutions — alongside newly minted college graduates. The student voices mattered deeply. They brought perspectives shaped not by policy debates or institutional legacy, but by lived experience. What I heard gave me pause.
In their words, trust in higher education is no longer assumed. As teenagers, they had known only polarization and sustained skepticism toward major institutions — including higher education. They questioned whether taking on heavy student debt is worth the risk.
Their reflections are a signal — and an invitation.
Design for the skeptical learner, not the ideal one
When trust erodes at this scale, the responsibility shifts to institutions to demonstrate value clearly, consistently, and transparently. Higher education must re-earn its place in people’s lives.
I found myself thinking about adults who have not yet reached higher education’s door — or who no longer believe college is meant for them. To reach the 75 percent aspiration, we must design for learners like those featured in a Strada Education video: working adults who are time-starved, balancing family and financial responsibilities, often cash-constrained, sometimes carrying eroded confidence in their ability to learn — yet keenly aware that they must keep pace in a rapidly changing world of work.
These learners remind me of Futuro Health Scholars. Their life circumstances are complex. Yet across our 41 education partners and 17 programs of study, they complete their allied health credentials at an 83 percent rate. The difference is not motivation. It is intentional design — structured supports, employer alignment, and clear pathways to good jobs.
When we design for the realities of learners’ lives, trust follows.
Accept partial trust — and build from there
Important policy reforms are underway — new accountability tools such as scorecards, and financing models that shift risk by requiring loan repayment only when graduates earn above a defined income threshold. At the same time, the higher education community continues to wrestle with longstanding debates — liberal arts versus career education, rather than “and” — while navigating institutional constraints.
Perhaps the more pragmatic path forward is not restoring blanket trust overnight, but building trust in specific, demonstrable ways. For working adults like those in the Strada video, trust may need to be earned for particular use cases, populations, or outcomes. For example:
“We may not yet be trusted for social mobility writ large, but we can be trusted for helping working adults become occupationally relevant within 12 months.”
This would require making the norms of effective career education more visible and portable across institutions — whether learning occurs in a community college or a liberal arts university. These norms include deep employer partnerships, employer-valued credentials, “soft”/essential skills development, competency-based technical training, work-integrated learning (clinicals, internships, co-ops, apprenticeships), credit for prior learning, stackable credentials, and sustained career navigation supports.
When these elements are transparent and consistently delivered, trust becomes earned rather than assumed.
Lower the cost of being wrong
One of the strongest signals of trustworthiness is lowering the cost of being wrong.
In both AI and higher education, the most credible systems are not those that promise perfection. They are the ones that make experimentation safe, mistakes visible, and course correction possible — without catastrophic downside for the learner.
This is why the challenge before us is larger than any single institution. It is about strengthening the category itself — redesigning learning so that people can enter, exit, and re-enter across their lives without incurring unmanageable debt or irreversible consequences.
What society needs is an intentional learning system that supports continuous transitions over a 30-plus-year work span — not only early-career education, but accelerated pathways into mid-career mastery as AI reshapes entry-level roles. A system people can rely on not once, but repeatedly.
Trust, in this sense, is not restored through persuasion. It is rebuilt through use. When people come back a second time—and a third—that is legitimacy.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader and formerly served as Executive Vice Chancellor of the California Community Colleges.
Keeping the Ladder Up: Ensuring Allied Health Workers Can Keep Climbing

By Van Ton-Quinlivan, CEO, Futuro Health
Over the past five years at Futuro Health, I have watched thousands of our Scholars step into healthcare through allied health roles — Medical Assistants, Phlebotomists, Sterile Processing Technicians, Community Health Workers and more. For many, allied health is not the final destination. It’s often the first rung on a ladder toward a career in nursing, advanced clinical, or other higher-level credentials. Justice J. and Carsyn P. are just two of many Futuro Health Scholars who aspire to advance in their careers by becoming RNs. Their journeys, which began in allied health, were recently featured in a BBC documentary presented by the International Council for Nurses. Their stories are a powerful reminder of how critical these pathways can be. You can watch their inspirational stories here.
Recent reports in the news highlight a troubling shift that could make that healthcare career ladder harder to climb: the federal government’s decision to remove nursing from the list of recognized “professional degrees.” This technical change has sweeping consequences. Graduate-level nursing students — pursuing MSN, DNP, NP or similar paths — will now face dramatically lower federal borrowing limits. The generous caps that once recognized nursing as essential to the nation’s workforce have been replaced with a ceiling of $20,500 per year and a lifetime maximum of $100,000. Even more concerning, the Grad PLUS loan program, which thousands of nurses relied on to bridge tuition and living costs during clinical training, is being phased out for these programs.
The impact is immediate and deeply inequitable. Advanced nursing education may simply become unaffordable for working adults, single parents, career changers, and those from low-income or underrepresented communities. These are the very people who have historically used allied health roles as steppingstones to upward mobility. When financing collapses, the pathway collapses with it.
That worries me, because at Futuro Health we have seen firsthand how powerful these pathways can be. Many Futuro Health Scholars (like Justice and Carsyn) begin as MAs or CHWs, gain confidence and income, and later pursue LVN-to-RN bridges, BSN programs, or behavioral health degrees — each step transforming their careers and their families’ futures. Allied health roles work as launch pads. They bring talented people into the system, help them build experience, and prepare them for more advanced roles.
But if the federal ruling signals that nursing is no longer treated as a profession worthy of investment, we risk discouraging people not only from pursuing advanced degrees — but from entering allied health altogether. Without clear, affordable next steps, early-career roles may feel like dead ends rather than ladders.
Since our 2020 launch, throughout the pandemic – and every workforce challenge since – Futuro Health has stayed focused on expanding opportunities: tuition-free or low-cost training, flexible schedules, coaching, and partnerships that lead to real jobs. We will continue doing that, because the future of healthcare depends on widening, not narrowing, the pathway for those who want to serve.
This is a moment that calls for courage and collaboration. Let’s work together — policy leaders, educators, employers, and communities — to keep pathways intact that allow working adults to advance in their careers. The future of our healthcare workforce depends on the decisions we make today. We owe it to every aspiring caregiver to keep each important step of the ladder intact and ensure the climb is still possible.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader and formerly served as Executive Vice Chancellor of the California Community Colleges.
A Letter of Gratitude; Reflections of Futuro Health’s Mission

By Van Ton-Quinlivan, CEO, Futuro Health
One of the greatest privileges of my work at Futuro Health is hearing directly from our Scholars—each with their own story of perseverance, hope, and transformation. Their journeys remind us why we exist: to expand opportunities for adults who want to serve in healthcare but need a bridge to get there.
Recently, I received a letter from Futuro Health Scholar Shiela M., whose journey captures the very heart of our mission. Her story is one of courage in the face of setbacks, and her words moved me deeply. With her permission, I’d like to share her letter here in full.
Letter of Gratitude and Reflection
This milestone means so much to me because the road to this achievement has not been an easy one. After completing my nursing degree in the Philippines, life took me on a detour that placed my NCLEX-RN dreams on hold for years. There were times I felt uncertain, as if the momentum I once had was gone.
But in the midst of those challenges, Futuro Health became a beacon of hope. Through their scholarship and unwavering support, I was given the chance to refresh the knowledge I feared I had lost and to rebuild my confidence. That opportunity made all the difference. Because of Futuro Health, I was able to give my best in the VN program, graduate as valedictorian and summa cum laude, and most importantly—believe in myself again.
I cannot express enough how deeply grateful I am to Futuro Health for investing in students like me. Their commitment to uplifting and empowering aspiring healthcare professionals is life-changing. They didn’t just provide financial assistance; they gave me the courage to continue pursuing my calling, even when the path seemed uncertain.
Passing the NCLEX-PN is another milestone that reassures me that it’s never too late to rise again and follow our dreams. With this accomplishment, I now look forward to preparing for the NCLEX-RN with renewed determination, knowing that Futuro Health has helped me lay a strong foundation for this next step.
As I look toward 2025, I am filled with gratitude and pride, ready to finally say: I’m officially a Nurse – LVN. This achievement is not mine alone —it belongs to every person and every program, like Futuro Health, that chose to believe in me when I struggled to believe in myself. Thank you for choosing me.
To anyone who feels their journey has been delayed: please don’t lose hope. Delays are not denials. Your moment will come, and with the right support, you will find your way. I am living proof of that truth, and I owe so much of it to Futuro Health’s guidance and generosity.
From the bottom of my heart-thank you, Futuro Health, for opening doors and helping me reclaim my dream.
With endless gratitude and determination,
Shiela M.
Licensed Vocational Nursing Program | Futuro Health Scholar | Valedictorian, Unitek College
Reading Shiela’s words fills me with both pride and humility. Her letter beautifully illustrates what we hope every Futuro Health Scholar experiences—a renewed sense of purpose and belief in their own potential.
At Futuro Health, we know that the path to a healthcare career is rarely a straight line. Life happens—detours, financial strain, caregiving responsibilities, and moments of self-doubt can make the dream of becoming a healthcare professional feel distant. That’s why we’re here: to meet learners where they are and walk alongside them as they reclaim that dream.
What moves me most about Shiela’s journey is her message to others: “Delays are not denials.” Those four words capture the spirit of thousands of our Scholars—individuals who persevere through challenge and emerge stronger, ready to serve their communities.
As we look back on 2025, I’m reminded that every milestone—every certification earned, every new healthcare role filled—represents not just a personal achievement, but a community impact. Each scholar we support strengthens the health and resilience of families and neighborhoods across our nation.
Thank you, Shiela, for sharing your story and for embodying what Futuro Health stands for: hope, opportunity, and the power to rise again.
Connected by Purpose: How We Built a Culture of Belonging from Miles Apart
By Van Ton-Quinlivan, CEO of Futuro Health
At a time when organizational leaders are wringing their hands over the future of remote work, our Futuro Health team has built something extraordinary — a culture that’s warm, inclusive, mission-driven, and deeply authentic, all without physical offices. This internal culture matters deeply, because it shows up in how we support the thousands of Futuro Health Scholars we serve — adults across a wide-range of communities who attend tuition-free to earn the credentials and qualifications they need to begin or advance their careers in healthcare.

By Van Ton-Quinlivan, CEO of Futuro Health
The U.S. is in the midst of a deepening mental and behavioral health crisis, with soaring rates of anxiety, depression, addiction, and trauma. But there’s a rising threat that’s often left out of the conversation as I have learned from my recent G7 Canada Brain Economy Summit participation: gambling addiction.
What was once limited to casinos is now as close as your smartphone. Americans are wagering nearly $1 billion a day on platforms like DraftKings and FanDuel. In 2024 alone, U.S. bettors spent an estimated $150 billion—a number driven higher by aggressive advertising and legalized sports betting in 39 states and D.C.
This surge is not without consequences. An estimated 2 to 4 million Americans will experience gambling disorder in their lifetime. One in six problem gamblers will attempt suicide. In Texas, despite strict gambling laws, calls to 1-800-GAMBLER are second only to California. In Pennsylvania, residents lost $238 million to online casinos in a single month.
And yet, gambling addiction remains a footnote in mental and behavioral health strategies, siloed from broader behavioral health initiatives.
A Workforce Ill-Equipped to Respond
The mental and behavioral health workforce is already stretched thin. According to Mental Health America, the U.S. has just one mental health provider per 350 people, and more than 152 million Americans live in designated shortage areas. This shortage is especially acute in rural and underserved communities.
When it comes to gambling-specific treatment, the numbers are even more alarming:
- Minnesota has just 8 certified therapists to serve an estimated 250,000 residents with gambling issues.
- Texas, home to 30 million people, has only three certified gambling counselors in spite of having the second largest call volume into 1-800-GAMBLER.
We need a workforce strategy that reflects the full landscape of mental and behavioral health, including gambling-related harm. And, we need to strengthen the pipeline not only for licensed professionals but also for the vital certificated roles that provide upstream prevention and support in mental and behavioral health.
What Can Be Done?
At Futuro Health, we work with states to strengthen the behavioral health talent pipeline, especially in under-resourced communities. Here’s what we advocate for mental and behavioral health workforce development:
- Upskill existing clinicians by embedding gambling-specific training into continuing education. Certifications like NCGC-I/II are already available and should be scaled.
- Grow certificated roles like Peer Support Specialists, Community Health Workers, Substance Used Disorder Specialists, and addiction-informed financial counselors. These roles can be trained faster and play a vital role in detection and early intervention.
- Grow talent from affected communities—especially rural, low-income, and minority populations where gambling harm is often highest.
A Call to Action
As was highlighted at the G7 Canada Brain Economy Summit, gambling addiction is not a niche issue—it’s a rising public health concern that warrants integration into our mental and behavioral health response.
Addressing Healthcare Worker Shortages: Insights from Keynote Speaking Across States
By Van Ton-Quinlivan
Connecticut, Texas, New Mexico, California, Nevada, Wyoming, New York – This month, I added Florida to the list of states where I’ve had the pleasure of delivering a keynote on the critical shortage of healthcare workers and raising visibility on the imperative to grow untapped talent from within our local communities. Even with the distinctive personalities and cultures of each state, the challenges they face are remarkably similar. Nationwide, 75% of healthcare facilities report critical workforce gaps, and 76.6M+ Americans live in designated Health Professional Shortage Areas. Across these in-state engagements, I offer organizations an alternative and innovative approach for growing their talent pool effectively. My key message? Rather than tackling the challenge alone, workforce development is, after all, a team sport. There is power in partnership.
100 Episodes of WorkforceRx: Insights, Innovation, and Impact

By Van Ton-Quinlivan, CEO, Futuro Health
When I launched the WorkforceRx podcast to spotlight leaders shaping the future of work, learning, and care, I anticipated gaining valuable insights—but the journey has exceeded expectations. Podcasting has not only been a platform for sharing ideas but also a catalyst for expanding my thinking and deepening my understanding of workforce innovations. Now, at 100 episodes, I’m reflecting on the game-changing ideas and inspiring voices that continue to shape how we future-proof our nation’s workforce.
A Front Row Seat to Workforce Innovations
In today’s rapidly evolving work environment—more VUCA (volatile, uncertain, complex, and ambiguous) than ever—traditional workforce models struggle to keep pace. Through WorkforceRx, I’ve had the privilege of speaking with leaders who aren’t just reacting to these challenges but actively shaping bold solutions.
They’re pioneering innovative funding mechanisms, redefining economic paradigms through modern co-ops and economic floors, and establishing apprenticeship degrees and alternatives for growing talent, while driving policies that scale workforce solutions—ensuring both workers and businesses thrive.
From AI-driven disruptions to reimagining primary care delivery and tackling behavioral health workforce shortages, these conversations underscore a key truth: adaptability is the new currency of success. Organizations that embrace continuous learning and agile workforce strategies will lead the future.
These lessons also apply to Futuro Health.
Embracing Agility While Standardizing for Impact
In just five years, more than 10,000 Futuro Health Scholars have earned credentials and qualifications to launch or advance careers in healthcare. By applying best practices in new ways, we’ve refined education pathways that unlock opportunities for untapped talent in diverse communities.
From recruitment and success coaching to essential and technical skills development, clinical externships, and the strategic use of data and technology, we’ve deepened our impact while standardizing processes for greater efficiency and scalability.
Connecting Systems Through the Power of Partnerships
Workforce development is a team sport, not a solo effort. No single entity can solve talent shortages alone—it takes collaboration among employers, educators, policymakers, funders, and communities to drive real change.
What if there were no wrong door for individuals to build skills and achieve economic mobility? That’s the possibility we’re working toward—one that demands collective action, shared innovation, and system-level transformation.
As we celebrate 100 episodes of WorkforceRx, I look forward to continuing these important conversations and forging new approaches to foster a resilient, future-ready workforce.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
Allied Health Roles & The Primary Care Doctor Shortage

By: Van Ton-Quinlivan, CEO, Futuro Health
The U.S. should expect a shortage of 64,000 physicians by year-end with the deficit growing to 86,000 by 2036, according to a McKinsey & Company Report. One third- of Americans lack access to primary care. These factoids headlined the recent California Healthcare Foundation panel that I participated on entitled “The Future of Primary Care.” Facilitated by Dr. Alan Glaseroff (Stanford Clinical Research Center of Excellence), I joined Dr. Megan Mahoney (UCSF Health) and Dr. Jay Lee (Integrated Health Partners of Southern California) to examine the implications of providing care when there are not enough primary care doctors to go around. All fingers point to a future where the approach shifts to a primary care team-based approach. No longer will the patient assume that every visit with the “doctor’s office” includes seeing the same primary care doctor; you may instead see members of an integrated care team that involves primary care, specialty care, and social services staff. For allied health level roles, this may include the medical assistant, the community health workers, and more…it just depends. The hope is to move from episodic visits – e.g., every few months if you have a condition — to more continuous care as the team leans in to monitor and act on your care needs and provision a “continuous healing relationship” as one speaker referenced.
For the Medical Assistant (a common and ubiquitous occupation), this team-based approach will require more training for expanded and flexed roles. The agility to cross-training MAs to rotate through multiple roles with add-on skills will become in-demand. Depending on the site, they may also need to be a phlebotomist, limited license radiologic technician, pharmacy technician, receptionist, greeter, referral coordinator, post-visit health coach, or medical clerk. Every team may need some combination of skillsets and certifications rather than singularly-trained roles. For more details, see Table 2 New Roles for MAs, Skills and Training Requirements in the article New Roles for Medical Assistants in Innovative Primary Care Practices.
This future of physician scarcity and dependency on a team to provision care is exciting to Futuro Health. We are offering the basics now and creating personalized education journeys that meet learners where they are – regardless of their prior education. Our education journeys bundle Success Coaching, Human Touch Healthcare, and a menu of one or more 17 technical programs of studies that lead into a healthcare credential (in partnership with our education provider ecosystem).
What if we could enable a future where employers, site by site, could select how they want to grow their allied health workforce for this team-based approach by custom designing which of credentials and specialty micro-credentials their workforce should have.
The future of primary care requires an extremely agile workforce development capability to keep up with foreseeable physician shortages, an aging patient population, and population growth without insurance coverage.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
Going for Gold: AI, Apprenticeships, and Shaping Workplace Champions
By: Van Ton-Quinlivan, CEO, Futuro Health
Like millions of others around the world, I spent the past two weeks captivated by the Paris Olympics, watching the incredible achievements of these highly trained athletes. The competition was a testament not only to their extraordinary skills but also to the profound influence of technology on sports training. With numerous world records being shattered, I found myself intrigued about how technological advancements are redefining the way athletes train and prepare, particularly with the growing role of artificial intelligence.
A quick internet search provided answers, uncovering numerous examples of how the sports industry is leveraging artificial intelligence to transform training, performance, and predict outcomes.

In my past blogs on the subject of generative AI in the workforce, I expressed my excitement for exploring applications of this technology to advance the future of learning and to unlock upward mobility in the workforce. Today, it is evident that the future is here. AI is making significant strides in every sector and industry (even among top-performing Olympians).
During a recent dinner table debate with my son (a newly minted college graduate), AI was once again a topic of discussion and whether it would eliminate entry level jobs that would have gone to new workforce entrants like him. He thinks all jobs suitable for recent college graduates will be done by AI in the future — and bases this foresight on his own use of ChatGPT 4.0 features.
I am not as bullish as he is but can see his point. Whether coding, building a website, writing manuals, running a spreadsheet, or solving math problems (particularly with the python integration), workplace tasks currently done by new college graduates foreseeably can be done faster by the AI.
I myself use the free version of ChatGPT and love how the tool makes completing certain tasks so much easier, including the task of writing job descriptions. Upon suffering two weeks of writer’s block, I took the advice of a colleague to use ChatGPT to generate a first draft. Voila! In less than one minute, it completed my HR task nearly perfectly. Soon after, I was asked to review several pages of web content to see if it captured us as an organization. Out of curiosity, I queried ChatGPT, and what it generated was an incredible set of succinct and clear bullet points that greatly improved the original draft. In these two small moments, I changed the nature of what entry-level analysts do in human resources and in communications departments.
Today many Fortune 500 companies are coming to this same conclusion about AI in the workplace, as it becomes integral to maintaining competitive advantage and staying relevant in an increasingly automated global market. Just this week JPMorgan Chase introduced a generative AI assistant to tens of thousands of its own employees, marking the first step in a larger initiative to integrate this technology across the vast financial institution. The program is now accessible to over 60,000 employees, assisting them with tasks such as drafting emails and reports. According to insiders, the AI software is anticipated to become as widespread as the videoconferencing tool Zoom.
So, with the adoption of new AI technologies, what’s a new college graduate to do to allay concerns and future-proof their career?
My WorkforceRx podcast guest, Vinz Koller at Social Policy Research Associates says, “The future of learning is work.” He advocates that apprenticeship training models where the individual is employed while simultaneously learning is the way forward. Vinz stressed the importance of transforming employers from mere consumers of talent into co-producers of talent, highlighting the need to demonstrate to employers how apprenticeships work and their benefits. Effective apprenticeship programs can lead to lower turnover rates and enhanced patient care. Listen to my compete interview with Vinz Koller here.
In an earlier podcast, I sat down with Ryan Craig at Achieve Partners, who authored the book, Apprentice Nation: How the ‘Earn and Learn’ Alternatives to Higher Education Will Create a Stronger and Fairer America. During our discussion, Ryan highlighted the benefits of apprenticeships for healthcare and hospital employers. He emphasized that paid apprenticeships eliminate employment uncertainty for workers by ensuring they are hired from the start. For employers, apprenticeships reduce friction by allowing hospitals to assess talent before making a final hiring decision. This way, both parties benefit: workers gain job security, and employers avoid hiring unproven talent. My entire discussion with Ryan Craig can be found here.
As we have seen with the successes of Olympic athletes who blend innovative technology with rigorous training, the same principles can apply to career development. By becoming lifelong learners and integrating into work environments that value both human ingenuity and technological innovation, the next generation can navigate the challenges ahead and emerge stronger, more resilient, and ready to thrive in a world where AI isn’t a threat, rather just one of many new tools at their disposal.
Reshaping the Mental and Behavioral Health Workforce

By: Van Ton-Quinlivan, CEO, Futuro Health
Mental Health Awareness Month arrives with a poignant reminder of the growing shortage of mental and behavioral health workers. This dearth not only affects the professionals themselves but casts a long shadow over patient care and community well-being.
I have spotlighted this critical issue in my past blogs, sharing strategies in behavioral health workforce development aimed at reducing stigma and enhancing access to mental health services. But too often these efforts face additional obstacles, particularly for behavioral health employers and workers in traditionally underserved, ethnically diverse, and rural communities.
A recent U.S. Government Accountability Office (GAO) study highlighted examples that in rural areas around the country, there is a shortage of licensed supervisors and internship positions needed to attract new workers. Additionally, behavioral health providers in rural communities often experience professional isolation, limited resources, and lengthy travel distances, exacerbating the need for more mental health workers, and making it challenging to deliver comprehensive care and support to patients in need.
Sharing our Best Practices
Futuro Health’s nonprofit mission is to improve the health and wealth of communities by growing the largest network of allied healthcare workers in the nation. We make education journeys into allied health careers possible by growing the talent that employers need and creating a path to opportunity that workers want. Our highly supportive education programs have enabled thousands of diverse Scholars to transition successfully into healthcare careers regardless of their educational background. The ethnic diversity of Futuro Health Scholars is now 90% and their linguistic diversity at 50% – with an average age of 31.
Our leadership team frequently shares our collective expertise and best practices in workforce development with renowned organizations like the World Health Organization, the National Governors Association (NGA), the Centers for Medicare and Medicaid Services (CMS), and various national, public, and employer groups. These include the Connecticut Workforce Summit, the New Mexico Hospital Association, the Texas Workforce Commission, The Healthcare Management Academy, and more.
Last year, Futuro Health was invited to participate in the National Governors Association’s Healthcare Workforce Project, a learning collaborative to support governors’ offices across the country in implementing strategies to strengthen and grow the next generation of the healthcare workforce by exchanging ideas and sharing best practices from national, state, and local experts. At the kickoff session, I was invited to speak to senior state officials from 20 states including Colorado, Missouri, Utah, and Wyoming on a solutions framework for tackling workforce challenges.
And in conjunction with Mental Health Awareness month, I am looking forward to leading a panel discussion later in May on the mental and behavioral health workforce challenge at the California Workforce Association’s 2024 WORKCON: Bridging the Gap with fellow panelists Anthony Cordova and Rehman Attar, respectively, from the California Community Colleges and California State University systems to speak on new public funds as well as the creation of a brand new occupation, called Wellness Coaches (see Related Readings at the bottom of this blog), to fill the missing rungs of the mental and behavioral health workforce ladder.
The State of Mental Health: Wyoming and Beyond
Forbes Advisor recently released its 2024 list of The Worst States for Mental Health Care. One in five adults experience a mental health condition each year. Of those, according to Mental Health America, more than half (54.7%, which is an estimated 28 million people) do not receive any treatment and more than one in four individuals (28.2%) do not receive adequate treatment, due to issues related to access to mental health care, worker shortages, and excessive costs.
Considering this alarming data, states like Wyoming are taking measures to proactively reform their state’s mental health system, and increase access to care through innovative programs like Wy We Care, a collaboration between the three branches of Wyoming’s government, the private industry, and philanthropic partners.
In our partnership with the National Governors Association, I am pleased to share that Futuro Health has begun exciting work to assist the state of Wyoming map educational pathways to address the shortage of behavioral health workers with a focus on growing the certificated workforce and identify stackable credentials. This effort aims to bridge workforce gaps and includes outreach to providers in Health Professional Shortage Areas (HPSA). While Futuro Health focuses on the education pathways to bring Wyomingites to enter these roles to serve their citizens, the Governor’s Office concurrently considers policies related to reimbursement of services to ensure the sustainability of these roles.
Investing in Success
Funding is critical to support the development of comprehensive education and training programs for mental and behavioral health workers, ensuring they have the knowledge, skills, and competencies needed to provide effective care. Recently, the U.S. Department of Health and Human Services (HHS) and the Substance Abuse and Mental Health Services Administration (SAMHSA) announced $46.8 million in funding opportunities to bolster youth mental health, expand the behavioral health workforce, enhance access to culturally competent care nationwide, and strengthen peer recovery support.
Similarly, the California Department of Health Care Access and Information (HCAI), is investing over $15.6 million in scholarships to support behavioral health students across the state and $120 million to create new Wellness Coach (Levels I and II) roles, initially supported through grants but intended to be reimbursable in the outyears.
As chair of the HCAI California Healthcare Workforce Education and Training Council, I have observed a pattern that clinical work experience remains a recurring barrier to growing the needed workforce. Upon listening to public feedback, HCAI revised its requirement for Level l Wellness Coaches, reducing the mandatory clinical hours for this role from 400 to 150. Now, individuals can be hired on a probationary basis upon completing 150 hours, allowing them to continue building their competencies while being paid and accrue the remaining hours needed to get to 400 total hours. This small change will invite more inclusive participation since few people can afford to go unpaid.
All the above are part of a broader initiative to strengthen California’s mental and behavioral workforce and emphasize the importance of a comprehensive approach to investing in systematic approach for establishing and stacking credentialing to grow workers and facilitate their upward mobility. This not only attracts more individuals from diverse communities into the field but ensures they possess the essential skills to deliver high-quality mental and behavioral healthcare.
Even as these examples provide promising models to grow the workforce, sustainability comes when there is a reimbursement model in place for mental and behavioral health services.
As we observe Mental Health Awareness Month, let’s shine a light on the critical need for more mental and behavioral health workers. By addressing the workforce shortage, we can improve access to care and enhance the well-being of individuals and communities.
* Related Reading: California Introduces New Wellness Coach Program Aimed at Building a More Diverse Behavioral Health Workforce to Help Children and Youth

By: Van Ton-Quinlivan, CEO, Futuro Health
As employers know, we are in a serious healthcare workforce shortage. According to AMN Healthcare, 85% of employers report Allied Health Staff shortages, and the American College of Healthcare Executives reports that workforce shortages topped the list of hospital CEO’s biggest concerns for the third year in a row. This shortage won’t resolve anytime soon. Experts project a 3.2 million shortage by 2026. The U.S. BLS tracks that resignations among healthcare workers have increased steadily from about 400,000 per month in 2020 to nearly 600,000 per month in May 2023. The recently released NHA 2024 industry outlook research report outlined similar concerns.
NHA’s report finds that workforce shortages are inspiring employers to embrace models of training and upskilling their workers to improve retention rates. In fact, over 70% of employers either have or are planning new hire or reskilling training programs to address staffing needs. NHA found that 82% of employees believe career laddering programs for entry-level workers would increase employee retention rates, and 71% of employees believe certification is very important/important to employee retention.
Employers have been engaging in clever practices to maintain costs and improve retention while maximizing people internally. Take the example of Pallas Care, serving residents of Los Angeles County, the agency employs state-registered home care aides to provide personal care management that help their clients maintain their independence and age with dignity. Pallas Care enrolled its staff of home care aides in Futuro Health CalGrows direct care worker training courses, which included Futuro Health’s Human Touch Healthcare™.
Rich Harvey, executive director and co-founder of Pallas Care, expressed how well Futuro Health’s culturally competent care and Human Touch Healthcare(tm) training aligned with his agency’s mission, values and goals.
Nurturing a diverse and resilient healthcare workforce

Last October, I was a part of a global panel put on by Women in Global Health, related to their report on why women in healthcare positions are resigning at concerning rates. Given the high proportion of females who comprise the healthcare workforce, this should be alarming to all.
As all healthcare providers know, retaining the current workforce holds primacy. Losing a nurse trainee within their first year of employment is a tragedy of investment – time and money invested by all parties, from the individual to the institutions that trained them and the employers who provided the clinical rotations. In my upcoming WorkforceRx podcast, CEO David Jarrard of Jarrard, Inc., a strategic healthcare communications firm whose clientele includes 1000+ healthcare employers, highlights how employers are reviewing the big and small in the daily routine of employees to fix sources of dissatisfaction. Issues range from scheduling, the ready availability of consumables to perform a job task, to job training and career pathing.
We are heartened to hear about employer’s retention efforts as we undertake Futuro Health’s work to bring untapped talents in communities into roles in healthcare. And, we expect our Scholars to persist and thrive in the industry. Since our organization’s inception, Futuro Health enrolled over 8,000 Futuro Health Scholars onto unique education journeys that lead them into healthcare credentials valued by employers – at low or no cost. We address the critical shortage in the allied healthcare workforce, and Futuro Health Scholars gain the opportunity to move into healthcare in good roles like phlebotomists, medical assistants, pharmacy techs, surgical techs, and more.
Interestingly, it’s the resiliency of our Scholars that impresses and will be an asset for an industry that articulates the importance of health equity. Listen to the stories of Futuro Health Scholars:
Everything everywhere all at once: the proliferation of healthcare worker shortages

We need to own up to some hard truths. It’s getting dire out here. There are pervasive shortages in healthcare workers across the spectrum. It doesn’t matter what state or country you’re in, or what field – there is a shortage of these essential workers.
It was a pattern I heard while speaking at the World Health Organization and the National Governors Association and something I observed in my role as chair of the California Workforce Healthcare Education and Training Council.
Just look at California alone. Does California have a shortage of primary care doctors? Yes. A shortage of specialty nurses? Yes. A shortage of workers in allied health roles? Yes again. How about a shortage of workers in oral health roles? Yes. And what about a shortage of mental and behavioral healthcare workers? Yes, in this field as well. However, California is not the only place experiencing this. In fact, California is a microcosm of this trend that is not only national but global as well.
In the U.S., “On the mental and behavioral health front alone, it would take 77,000 more school counselors, 63,000 more school psychologists and probably tens of thousands of school social workers to reach levels recommended by professional groups before the pandemic hit,” according to a recent article in the Washington Post. “Typically, the jobs require a master’s degree, meaning six or seven years of higher education. The pipeline does not flow rapidly.”
In the meanwhile, communities – from children to adults – struggle.
Even maintaining the existing workforce is not enough. As the population ages, the demand for care and caregivers also increases. In 1950, there were 11.7 working-aged people for every person over the age of 65. Today there are only 7. And worse, by 2040, this number is expected to shrink to 4.4. That is not sustainable.
By 2050, the population that is 65 and older will more than double. This older population will grow from 9.4% to 16.5% of the total population. It is projected that 40% of in-home care is provided by family members, many of whom are thrust into this role. As demands for care increase as the population ages, it will further challenge our nation’s already limited supply of healthcare workers in the workforce. If we continue this path, who will care for our family when they get sick? Or for us when we age?
We know there are untapped talents wanting the opportunity to work in healthcare. Our focus groups showed they did not know how to enter the field, and those who managed to do so incurred too much debt. Futuro Health recently announced a new $100 million commitment from Kaiser Permanente to expand our services nationwide beyond California, including Colorado, Oregon, and Washington, to continue this work.
Our mission is to improve the health and wealth of communities by growing the largest network of allied healthcare workers in the nation, and we do that by making education journeys into careers in healthcare possible through growing talent for employers and connecting workers to opportunity. At Futuro Health, we are facing the allied healthcare workforce shortage everywhere and all at once head-on.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
Thanksgiving Reflections on Partnerships, Progress, and Futuro Health's Journey
By Van Ton-Quinlivan, CEO, Futuro Health
As we observe this Thanksgiving season, I am grateful on so many fronts.
We appreciate our Scholars: Futuro Health has touched over 9,000 lives since our launch four years ago. We see our impact in their smiles (see graduation photo) and their personal stories. With 85% of healthcare facilities reporting a shortage of allied health workers, the call to action is great to unlock talent who otherwise would remain untapped. We are so proud of all our Scholars who embarked on personalized education journeys toward their in-demand healthcare credential.
We appreciate our partners. I often write that workforce development is a team sport. No one of us can do everything on our own. Our thanks go to our ecosystem of 20 education partners including community colleges and 4-year public institutions, our employers and funders who provide no- or low-cost education journeys through us, and our board members who guide our organization’s mission to improve the health and wealth of communities by growing the largest network of allied healthcare workers in the nation. This Thanksgiving season holds a special significance as we express our gratitude for the new $100 million commitment to expand our impact across the country to address the nation’s critical staffing shortages.
We appreciate the Futuro Health Team. We have an amazing team. They bring their gifts to bear so that we can do our transformative work with Futuro Health Scholars. I am so thankful for their hard work and dedication and the support they each receive from their loved ones to do this purpose-driven work.
I wish you a wonderful Thanksgiving!
The Future of Aging and Automation

I just returned from a Future of Work design thinking workshop hosted by IDEO and Blue Meridian Partners in NY. An intimate and diverse group of participants, all experts in their domain ranging from workforce development to social impact investing, were taken through a set of immersive scenarios that described how work could manifest 15 years from now based on the impact of technological advancements like AI. This type of futures-thinking workshop prods participants out of their comfort zone and serves as a good tool for ideation. Similar to other future of work discussions in which I have participated, caregiving came up as a set of occupations that would persist – care for the young, the elderly, the sick, the disabled, and the community – rather than be fully automated. While on the surface, that sounds promising, Paurvi Bhatt, board member on the Rosalynn Carter Institute for Caregivers, forewarned when she appeared as a guest my WorkforceRx podcast,
The Healthcare Workforce Crisis. Are Students Drowning in Debt or Is the Industry Under-Selling Its Jobs?

By: Van Ton-Quinlivan
Education and training are requisites in the highly credentialed field of care. Nowadays, however, it is difficult to avoid news surrounding the burden of student debt and the long-term consequences it imposes on borrowers. With punitive interest rates reaching as high as 15% annually, it’s not uncommon to hear stories of students who graduated with five-figure student loans, which can put things like homeownership and a better life out of reach. I recently reviewed student debt data for California and was shocked by the increase to an average of $37,084 student debt in 2022, up sharply from $21,125 during the 2019-20 pre-pandemic years. Curious about the broader picture, I researched national student debt figures, only to verify that California is not an anomaly, with the average student debt across all 50 states being comparable during this same time.
With the temporary relief of the three-year freeze on student loan interest and payments coming to an end this fall, shifting the conversation from providing temporary student debt forgiveness to a more comprehensive exploration of long-term solutions can aid the field of healthcare where skilled workers are in short supply.
The Ripple Effects of Rising Student Debt
Student debt, combined with overall cost-of-living increases, has had an impact on the average savings account balances across different racial and ethnic groups, with a disproportionate burden of student debt among Black and Hispanic students compared to white borrowers. According to data from the Federal Reserve, this stems from various factors, including systemic inequalities, limited access to resources, and a higher likelihood of attending for-profit institutions with higher tuition costs.
Given how enrollment in universities and community colleges have trended downward during and after the pandemic, states are offering up incentives – such as free community college – to entice learners to return.
For healthcare specifically, diversifying the workforce is a business imperative. Given that healthcare outcomes are shown to improve when those who provide care mirror the communities they serve, the sector is wrestling with how to address its skilled worker shortages. For individuals with the willingness to put in the effort to secure a better life and opportunity, debt is clearly a prohibitive barrier – we heard the same in our focus groups. And this need not be the case. By removing the ogre of adding to education debt thanks to our funders, Futuro Health has brought forth an otherwise hidden workforce into the field of care.
Take Ebonie C., a Futuro Health Scholar who recently completed tuition-free training as a Patient Care Representative. Ebonie spent years working the nightshift at local homeless shelters to provide for her family, never losing sight of her commitment to helping people. Ebonie grew up learning first-hand the importance of comprehensive patient care, having two parents who lived with amputations. Ebonie’s dream job is to be a wound care nurse, and today she is debt-free as a Futuro Health Scholar and one step closer to that dream as she explores new job opportunities.
Mental Health and the Healthcare Workforce Crisis

By: Van Ton-Quinlivan
During May, the nation observes Mental Health Awareness Month, dedicated to raising awareness, challenging stigmas, and advocating for mental well-being.
According to Mental Health America, one in five adults in the country suffers from mental illness. While behavioral health challenges affect individuals from all backgrounds and occupations, healthcare workers face heightened levels of stress, making them particularly susceptible to conditions such as anxiety, depression, and post-traumatic stress disorder.
Recently released government data indicates an alarming increase over the past three years of healthcare workers who have left or resigned their roles due to burnout and other mental health conditions, exacerbating the existing strain on healthcare providers. A study conducted by the National Forum of State Nursing Workforce Centers revealed that 100,000 nurses left the profession during the pandemic, and it is projected that up to an additional 800,000 nurses plan to retire by 2027 due to factors such as stress, burnout, or opting for early retirement.
The demand for healthcare professionals extends beyond the need for nurses. The shortage of allied health workers is at unprecedented levels, with one recent survey concluding that more than 85% of hospitals and health systems are experiencing a critical shortage of allied health staff. Currently, the allied healthcare sector accounts for approximately 60 percent of all healthcare positions in the United States, with the need for additional allied health workers only expected to grow by 20% through 2026.
A Perfect Storm
The exodus of experienced healthcare workers seeking respite from emotional strain, on top of normal attrition is creating a significant workforce gap, leaving healthcare employers facing staffing and retention challenges as remaining workers are burdened with increased workloads to compensate for the shortfall.
Why not bring in new graduates, you may ask? Shortages in the capacity to supervise new grads hinder a seemingly solid solution for curing this cycle. It’s an ongoing conundrum, as outsized cost pressures loom large for healthcare employers, yet many continue to hire travelers, often at two to three times the cost. In fact, reducing cost was a central theme as C-suite executives gathered at The Healthcare Management Academy in Nashville, where I recently spoke on the topic of workforce best practices. There is no fast, easy solution to today’s complex circumstances.
Care for the Caregiver
Futuro Health has brought thousands of diverse adults into education journeys along their way to allied healthcare careers, reflecting 90 percent diversity and with an average age of 29. Changing careers and returning to education can be a rewarding adventure for adults looking to reinvent themselves or pursue new jobs. However, it can also be a highly stressful and a mentally challenging experience.
One of the most significant sources of stress is the financial burden of returning to school. Adult students may need to juggle the high costs of tuition while also managing their living expenses. Additionally, many struggle to balance a job, family, or caregiving responsibilities while resuming their education, which can be extremely demanding on their time and energy. For any older adult, simply returning to school can be intimidating itself, particularly with coursework now online or hybrid.
Our staff at Futuro Health spends countless hours supporting our adult Scholars, and our unique model provides a solution to their challenges, including offering tuition-free training opportunities and pathways into careers in allied health, while our online approach to learning allows them the convenience of completing training remotely, often at their own pace, and with guidance from a dedicated team of Futuro Health Success Coaches to assist them all along their educational journey and prepare them for new careers. This includes our Human Touch Healthcare training, which provides the essential interpersonal skills to work in healthcare, encompassing such competencies as Empathy & Compassion, Effective Communication, Emotional Intelligence, Teamwork & Collaboration, and Ethics & Integrity.
Futuro Health is taking steps to assure we are mindful of the mental well-being of our team members and the Scholars they serve. As just one such example, John Cordova, RN and Futuro Health’s Director of Workforce Development & Externship, advocates for self-care and shared this useful link to Take Action for Mental Health (among other resources) within our organization to remind each of us to:
- Check in about mental health.
- Learn More about mental health needs and what you can do.
- Get Support for yourself or someone you care about.
By nurturing a lifelong resilience mindset and fostering a supportive network, we can all strive to create an environment that prioritizes mental well-being. Mental Health Awareness Month presents an opportunity to shine a light on the mental well-being of healthcare workers during May – and throughout the year – as we actively work towards building a more sustainable future for these compassionate individuals who dedicate their lives to caring for others.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
The Unique Role of an “Education Whisperer” in Workforce Development
By: Van Ton-Quinlivan
In the U.S., over 80% of healthcare facilities have reported a shortage of allied healthcare workers. This persistent workforce deficit necessitates collaboration between employers and higher education to find a solution. Yet, interpreting the languages between these two worlds can be a challenge. That’s where the need for an “education whisperer” comes in. Our team at Futuro Health fills this crucial role.
Crafting a “win-win” matters a lot in workforce development. Ask incoming California Community Colleges Chancellor Dr. Sonya Christian.

Dr. Christian, in her prior role overseeing a district of three rural California community colleges, she sought to increase participation of diverse communities in healthcare careers. Like the rest of America, her colleges were losing enrollment. According to the National Center for Education Statistics, higher education nationwide suffered from 7.6% less students enrolling in 4-year colleges and 16.2% fewer students in community colleges compared to pre-pandemic levels. Enrollment is the lifeblood of colleges. Creating costly new programs when there is enrollment uncertainty brings only risk.
Because Dr. Christian and I worked together during my time as Executive Vice Chancellor of California Community Colleges, we talked about engaging Futuro Health’s expertise to de-risk enrollment uncertainty for a community college in her district, Cerro Coso College, to launch a new hybrid Medical Assistant Program for rural communities. Futuro Health took on the role of education whisperer by encouraging Cerro Coso College to adopt best practices, such as decoupling from the academic calendar, to accommodate more adult learners. Together, our organizations worked through new data exchange and enrollment protocols to enable us to support working adults in their educational journey more seamlessly. The first cohort launched and was quickly filled. In turn, Futuro Health stepped in to engage with employers who provided qualified applicants for the hybrid Medical Assistant Program.
A Podcaster’s (Grateful) Perspective: What would ChatGPT Say?

Recently, we celebrated the release of the 50th episode of my podcast WorkforceRx with Futuro Health. As I reflect on this milestone, I am filled with appreciation for all the incredible guests and listeners who have been a part of this journey. My guests include a wide range of inspiring individuals with diverse backgrounds, including education, healthcare and business thought leaders, entrepreneurs, clinicians and many others. They readily shared their knowledge and experience as we probed innovations that ready us for the future of work, future of care and future of learning.
In preparing for this blog, I looked back at our first 50 podcast episodes and was struck by the number of issues we covered that have since gained national prominence – including workforce shortages, the adoption of skills-based hiring, burgeoning mental health issues, and strategies for inclusive economies. However, no topic has gained more attention recently than advances made in Artificial Intelligence (AI) and its impact in the workplace and classroom.
Today, chatbots like ChatGPT have thrust AI into the center of major debate and controversy, generating buzz and fear in equal measure for its ability to generate conversational text to produce anything from simple answers to elaborate essays, scripts, lyrics, and much more. If ChatGPT can generate a 1,000-word essay in under two minutes and solve a complicated math formula in one, it begs the question: What are humans for? Especially as technology becomes significantly refined in the future.
I had the privilege of interviewing one of the nation’s leading AI experts on my podcast, Dr. Tom Mitchell, AI Scientist and founder of the very first Machine Learning academic departments in the nation at Carnegie Mellon University. He addressed concerns that AI in the workplace will replace humans and make many current work functions obsolete. Experts like Dr. Mitchell contend that AI will create additional career opportunities through more collaborative relationships between workers and technology. “Humans paired with technology” was his phrase.
Since ChatGPT’s launch in November, those in academia have raised concerns it could facilitate cheating, and the response by educators has been swift and varied. Last week, New York City’s education department blocked ChatGPT on all school devices and networks, citing negative impacts on student learning, and concerns regarding the safety and accuracy of content. While in other states, educators are embracing the technology’s ability to improve student writing, helping them generate ideas and reimagine the writing process.
I gave ChatGPT my own test drive, asking it to produce responses to some rudimentary “how to” questions commonly asked in my field of workforce development – like What is workforce development? and How Do you create a public-private partnership? I was generally impressed with the resulting write ups generated by ChatGPT. Then, I wondered if it could generate podcast scripts (which would make podcast producers, including mine, quite unhappy), and could I feed it all 50 podcast transcripts to render a book that synthesizes themes, which could make developmental editors skittish.
My findings using ChatGPT confirmed for me what many of the AI experts featured on my podcast also concluded:
- The importance of emotional intelligence in the workspace cannot be overemphasized. Intelligence is one distinguishing factor that will assure that humans forever remain relevant in the workplace.
- Digital skills and digital access are so fundamental to maneuvering the future that those without both will not be positioned well in the economy.
- The rapid breakthroughs in technology will challenge how we train, adapt and adopt at a more rapid pace. All education and training modalities will need to continuously reinvent themselves, from higher education institutions to smart devices.
It wasn’t long ago that advances like cloud technology, data collection and video-based communications sparked its own wave of concerns about technology replacing humans in the workplace. Today, we can hardly imagine a work environment without these technologies. We not only adapted, but these advances in technology have ushered in entirely new career sectors and job opportunities.
Perhaps this is a good time to remember a quote from one of the founding fathers of technology, Steve Jobs, Co-founder of Apple, who said “It’s not a faith in technology. It’s faith in people.”
I look forward to continuing to host our WorkforceRx podcast and sharing my (very human) conversations with all of you for many more episodes to come.
Speaking Out - The Healthcare Workforce Crisis

Through our Futuro Health Speakers Bureau , I am frequently invited by employer groups, national organizations, and education- and workforce-based organizations from across the country to speak. At these conferences, symposiums, forums, and other events, I highlight best practices from my book Workforce Rx: Agile and Inclusive Strategies for Employers, Educators and Workers in Unsettled Times to inspire action. (Note: Proceeds go to benefit Futuro Health’s nonprofit mission). Although states have their differences, what they have in common is a shared pain around their shortage of healthcare workers. While the need for physicians and nurses has been widely publicized, the shortage of allied health workers too often goes overlooked.
According to new data, the allied health worker shortage has put employers in a highly precarious situation, with 85% of healthcare facilities facing unprecedented needs for allied health professionals. In California alone, the deficit of allied health workers is expected to increase to 500,000 by 2024. The demand for these essential workers, including medical assistants, pharmacy technicians, health IT specialists, EMTs, phlebotomists, peer support specialists, community health workers and more, has reached critical levels, adding to an already strained healthcare delivery system in the U.S.
My book drew from my years of experience in the private, public, and now nonprofit sector refining best practices in workforce development. Doing speeches to Wyoming, DC, NY, Connecticut, Colorado and California audiences helped me understand which workforce challenge, which stories, which solutions best resonates. Let me share with you what themes states have in common.
Aleki’s Story, A Fishing Tale
Recently I keynoted the Connecticut Workforce Summit, hosted by the state’s largest business organization, CBIA, and by Social Venture Partners. Like other states, Connecticut is facing significant worker shortages in many sectors, from manufacturing to healthcare. Mark Argosh, chair of Connecticut Governor Workforce Council (and WorkforceRx podcast guest speaker), estimates 109,000 job vacancies, which is more than the number of those unemployed in the state.
One-third of high school graduates in Connecticut do not go on to any form of higher education. Connecticut fortunately does prepare youths while they are still in high school for careers by collaborating with the state’s school systems to develop career pathways. Post high school, many are stuck in low-wage jobs and are prime candidates for upskilling. Others may have the necessary requisites but encounter problems navigating the search and hiring process. That population needs a different solution and employing industry sector strategies has enabled the state to do deeper work. On the sidelines, a large number of disconnected youths – estimated at 40,000 – are neither working nor attending school and need to be reengaged in order to supply the needed workforce.
Speaking to the Connecticut audience of mostly 500 business leaders and employers, I shared the story of Aleki from my book chapter entitled: Leveling the Slope of Unconscious Bias. During an earlier time in my career working in the energy sector, I launched and led the Pacific Gas and Electric PowerPathway(tm) workforce development program, where I met Aleki, an inspiring 19-year-old who was seemingly a good fit for an open position in our organization. Following the standard drug screen, background check and completion of a 3-month pre-hire training, we were perplexed as to why Aleki had fallen off the short list of candidates.
Upon making inquiries, we learned that Aleki didn’t pass his background check due to, of all things, an unpaid fishing fine he received at the age of 15 for catching a fish that was too small by local regulations. Aleki was unaware that his unpaid fine escalated up through the court system, leading to him being charged with a nonviolent felony. Fortunately, our community partner helped Aleki get his record expunged, and he got the job.
Aleki’s story serves as an example of why workforce development is a team sport between employers, education providers, and the workforce- or community-organizations, with each stakeholder doing what they do best, to enable the Alekis to enter the talent pipeline. The collaborative efforts in Connecticut – including career pathways, sector strategies, and a collaborative approach to workforce development – combine to put Connecticut in the right direction. Connecticut received in 2022 the largest federal Good Jobs Challenge grant award (nearly $25M) for its momentum.
The Robot Zombie Apocalypse and other Misperceptions
There have been many misperceptions related to workforce development, artificial intelligence (AI) and robotic process automation. For years I’ve been hearing about the coming of the robot zombie apocalypse, the speculative fear that AI and automation will replace humans in the future of work.
This past summer I was honored to speak on a panel about Automation and the U.S. Workforce, hosted by The National Academies, a private, nonprofit institution that provides expert advice on some of the most pressing challenges facing the nation and world, shaping sound policies, informing public opinion, and advancing the pursuit of science, engineering, and medicine. Carnegie Mellon University Dr. Tom Mitchell of the National Academies invited me to address its leadership body tasked with refreshing a report to Congress on the impact of AI.
I reflected on the views of leading experts from both private and public sectors, including Jamie Merisotis, CEO of The Lumina Foundation, and author of his own book: Human Work in the Age of Machines. Experts like Jamie agree that one of the things that differentiate humans from machines in the workplace is that for us as humans, work matters. AI lacks the softer skills to work in jobs that require critical thinking and creative approaches. Like Dr. Mitchell who espouses that AI will augment the workers (hear him speak on my podcast interview of him here), Jamie believes AI and automation do not pose a threat to the workforce as much as it will open opportunities for a more collaborative relationship between employers and technology.
To prevent the worker from being left behind with advances in technology, however, regular skills upgrades will be required. What states have in common is the challenge to bring down structural silos that hinder employers and education from working together more symbiotically. The chapter in my book entitled Making the Fire Hose and the Garden Hose Work Together advances the premise that education and employment can no longer operate independent of each other’s respective priorities. Employers need to form consortia to aggregate jobs across divisions, suppliers, adjacent industries, and competitors – and better match the economics of higher education to engage in creating up-to-date curriculum needed especially by working learners to keep pace with the workplace changes.
Uniting for Solutions
Perhaps one of the most impactful examples of collaboration I observed while on speaking across state lines comes from my participation earlier this year in the kickoff meeting of the National Governors Association’s (NGA) Healthcare Workforce Collaborative. The NGA is a bipartisan organization comprised of the nation’s governors, with a mission to share best practices and speak with a collective voice on issues of concern impacting all 50 states.
This kickoff NGA meeting marked the introduction of a six-month multi-state program collaboration aimed at addressing the healthcare workforce shortages in 14 states. By learning directly from other states and national experts, the participating states understood innovative policies, programs, and practices to create a positive environment for an enduring healthcare workforce.
In my keynote, I offered up solutions drawn from in my book to address what keeps healthcare CEOs and COOs up at night, touching on such issues as retention, cost, and reskilling challenges, as well as the desire to add diversity in new hires.
The lack of healthcare workers has become so prevalent across the country that more than 20 governors this year directly addressed the situation in their state of the state speeches, proposing a range of policy fixes and funding initiatives, including California Gov. Gavin Newsom, who recently announced a new plan to invest $4.7 billion to overhaul California’s mental health system by adding 40,000 new skilled workers in mental health fields.
This level of cooperation and rallying among states to find common ground solutions to the healthcare workforce shortage underscores my earlier point that the shortage has indeed become a national crisis, impacting those in every state.
During any crisis, it is human instinct to want to play defense. Instead, applying best practices in workforce development – as outlined in WorkforceRx – puts in place proactive tactics that equip an organization with the right skills at the right time. I am encouraged by the openness of the many groups I speak who are recognizing that this is the right time to reconceptualize staffing shortages as an opportunity among industry, education, government and regional organizations and providers to work together on a solution. Workforce development, after all, is a team, not individual, sport.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public, and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
What We Can Learn from Education Disruptor All-Star Sal Khan and His Innovations
I have the privilege of meeting many leading experts and innovators in the education and healthcare sectors in my role as CEO of Futuro Health (see some featured in my WorkforceRx podcast). Recently, I bumped into education icon, Sal Khan, in Silicon Valley. Sal is an education innovator all-star not only in my eyes but of many around the world. And, his latest creation, SchoolHouse.World.org, will infuse innovation into the college admissions process.
Sal does his global work on the second floor of a Google building in Mountain View, California. My youngest son enrolled in Sal’s experimental Khan Lab School, an in-person K-12 school located on the first floor of the same building, after the pandemic wreaked havoc with his schooling, as it did for many. Now a senior, my son is going through the college admissions process, which unfortunately in the U.S. is an all-too-stressful rite of passage.
Sal and two college admission directors hosted a discussion with students and parents. That was where I met him in-person. I had seen Sal speak over a decade earlier when he delivered a provocative keynote to a skeptical audience of national higher education leaders. I was inspired then by his notion that learning can be based on mastery rather than time-in-seat. Almost everything in higher education is anchored in the construct of time – a.k.a., the credit hour.
What Makes Sal Khan an Education Disruptor All-Star?
Mastery-based learning will no doubt become a best practice in the future landscape of workforce development as workers struggle to pace with the rate of technology ingestion. All of us will need more strategies to accelerate our attainment and demonstration of new skills.
Can we speed through what we have already mastered and spend more time on what we haven’t yet? Sal’s Khan Academy has shown what can be done. The learning tools developed in Khan Academy are used by 135+ million people from over 190 countries who pursue knowledge through mastery-based learning. Learners, upon demonstrating competency on a concept, can move ahead quicker.
The converse would also be true for learners who need more time. Student progress no longer is measured by the 50 minutes spent in the classroom and is decoupled from when the bell rings or calendar year ends.
Working the Problem Can Lead to Unintentional Innovations in Education
Back to Sal. With Khan Academy and Khan Lab School in full deployment, he is once again at work solving the dilemmas of education in novel ways. Sal now wants to provide free tutoring to the world in a new venture called SchoolHouse.World. His team had a dilemma to solve, “How do we know a person is qualified to be a tutor?” In working the problem, his team designed a process whereby applicants recorded themselves on video teaching a topic (e.g., in calculus), then submitting the recording for peer rating. Qualified submissions would earn a SchoolHouse.World certification.
Coincidentally, the pandemic came about whereupon colleges suspended their collection of standardized scores. Seeing the value of SchoolHouse.World.org certifications as a good indicator of what students knew, faculty at MIT, Georgia Tech, and the University of Chicago began accepting them in lieu of ACT and SAT scores – and, as such, introduced innovation into the archaic college admissions process.
Like the invention of the Post-Its by 3M, Sal’s innovation was accidental for he was focused on the K-12 space. Few people know that Post-It Notes were amazingly close to complete failure. In 1968, Dr. Spencer Silver, a chemist at 3M Company, invented a unique, low-tack adhesive that would stick to things but also could be repositioned multiple times. He was trying to invent a super-strong adhesive, but he came up with a super-weak one instead. 3M shelved the discovery for five years, until an opportunity arose for its use bookmarking and highlighting textbook pages without damaging them. Fast forward 50 years, and Post-It Notes can be found in offices and meeting rooms worldwide.
Embracing the Needed Innovation to Higher Education Practices
The story behind the invention of Post-It Notes is a favorite example of how experimentation often leads to unplanned discoveries. Sal’s college admissions innovation came about when he sought a solution for something else.
Since launching in 2020, Futuro Health benefitted from having a whiteboard in which to approach developing the allied health workforce. We have uncovered novel ways to organize community organizations and unions to efficiently scout diverse adults and being them onto education paths. At a moment in time when higher education enrollment nose-dived across the nation, especially in 2-year institutions, Futuro Health has met and exceeded our goals for how many students we serve each year. We are infusing some of those learnings into our collaboration with our public institution partners, including California community college, California State University and University of California brethren, who join us in a federal grant to grow the state’s public health IT workforce called California Consortium for Public Health IT (CCPHIT).
As I look back on my recent encounter with Sal Khan, I am reminded that innovations come about in so many ways.
Futuro Health CEO Van Ton-Quinlivan is a nationally recognized expert in workforce development. Her distinguished career spans the private, public and nonprofit sectors. She is a White House Champion of Change and California Steward Leader, and formerly served as Executive Vice Chancellor of the California Community Colleges.
Filling the Mental Health Worker Pipeline Amid a Growing Crisis
By Van Ton-Quinlivan, CEO Futuro Health
You don’t have to look further than the daily news headlines to be reminded that we are facing an unprecedented mental health crisis in our nation. The unfortunate aftermath of COVID-19 has resulted in a subsequent pandemic impacting the mental and behavioral health of those in communities across the country, and the numbers are alarming.
According to new data from the National Alliance on Mental Illness (NAMI), one in five adults in America experience a mental illness and nearly one in 25 adults live with a serious mental illness. And, perhaps even more startling, one-half of all chronic mental illness begins by the age of 14. In some instances, this equates to a 25 percent increase in those being diagnosed with behavioral health disorders when compared to pre-pandemic levels.
There have been numerous studies on the pandemic’s impact on the state of mental health in America, many citing isolation, disruptions to schools and businesses, and limitations placed on in-person health care services as contributing factors to the current mental health crisis. While the pandemic was undoubtedly a tipping point in the escalation of mental health diagnoses, behavioral health experts have been warning of looming disruptions for mental health providers for years prior to the repercussions of COVID-19, including job burnout, availability of training, lack of opportunity for minorities, an aging workforce and retirement drain.
These factors become compounded when considering that mental health services have historically been difficult to access in rural communities, where healthcare choices are more limited than they are for residents of cities and suburbia. And for those hoping to find a Black or Spanish-speaking therapist, their options are even less, resulting in significant disparities in care for those who need it most, all of which has only been exacerbated by the aftermath effects of the pandemic.
A Skilled Workforce: Building Blocks to a Solution
It’s difficult to solve the big issues when there are missing pieces to construct the solution. A key piece is always the workforce necessary to do the work. A skilled workforce is one of those building blocks that enables and, when not available, certainly hinders progress.
The lack of mental health workers isn’t confined to rural America. In California this week, the San Diego Workforce Partnership issued its own call to action by highlighting the importance of adding more skilled workers as a solution to the mental and behavioral health issues within its own densely populated county lines.
The Workforce’s new report: Addressing San Diego’s Behavioral Health Worker Shortage, emphasizes the need to fill the mental health worker pipeline by educating, training, attracting, employing, and retaining 18,500 additional professionals between 2022 and 2027 to meet the anticipated behavioral health and addiction treatment needs for residents of San Diego County. According to the report, the worker shortage in San Diego County spans a range of titles, some trained through certificates that can be attained under one year, while others require advanced degrees.
Barriers to Mental Health for Racial and Ethnic Minority Groups
Research has shown that racial and ethnic minorities have significantly less access to mental health services than others, and thus are less likely to receive proper care and treatment. Many of these same studies show that one of the best ways to improve health outcomes in underserved communities and among minority populations is to ensure that the medical professionals not only serve their communities but are representative of their communities they serve.
At Futuro Health, we place critical importance in helping students get a tuition-free education in healthcare roles that are in-demand and impactful, filling the gaps caused by differences in income, education, race, ethnicity, and location. Since our launch in 2020, Futuro Health has successfully brought over 8,000 adults back into higher education, with 80% diversity, to train at our partner colleges.
Microcredentialing: A Responsive Solution for Leveraging Untapped Talent
Solving Workforce Shortages is Not an Individual Sport: What Healthcare Needs to Do Differently
by Van Ton-Quinlivan, CEO of Futuro Health and Jeff Weiss, Founder and Managing Director of Center for Corporate Innovation (CCI)
We all know how deep and severe the demand for nurses and allied health workers grew over the course of the pandemic. We still live it. From the skyrocketing cost of traveling nurses to retaining those who are burnt out and frustrated, from sourcing diverse hires for better health outcomes to reskilling current employees for technology changes, to addressing how telework impacts culture and employment tenure, these challenges facing the healthcare workforce keep CEOs up at night. Many of you share in their struggle and seek to find solutions.
How do we fill vital allied health roles in a reliable and inclusive way? Allied health roles comprise an estimated 60% of the care workforce. They run the gamut of occupations including medical assistants, phlebotomists, vocational/practical nurses, sterile processing techs, surgical techs, health IT and data analysts, peer support specialists, community health workers, and so on.
According to pre-pandemic numbers, the United States will need an additional 2.3 million allied healthcare workers by 2025, and California alone will need 500,000 of them by 2024. Numbers this large mean the challenge is structural, and no one organization can realistically take on the challenge alone.
One proven solution is through industry collaboration: working together to source, support, and train a diverse talent pool so they have the right skills at the right time. It’s often tempting for healthcare employers to try and build their own workforce solution. Forming a consortia can feel like an anathema for healthcare systems that normally compete. However, reaching out to partners and forging a path of collaboration can make a stronger workforce pool and one infused with more diverse talent.
Grouping employers into a consortia is a workforce best practice. Bringing together peers, suppliers, adjacent industries, and even competitors in order to bring forth solutions at a level of scale to mirror the size of the issue can have outstanding results. Once employers form into a consortia within a region, education and public sector resources can more efficiently liaison and braid to meet the labor market needs.
This playbook comes road tested. The nation’s electric, gas, and nuclear sectors (for short, we’ll call it the energy sector) went through a similar metamorphosis in the early 2000s when it foresaw 25-50% of workers on the verge of retirement. Like the aging of seasoned nurses in healthcare, energy employers foresaw the exodus and ushered in a whole set of strategies based on collaboration. State-by-state, employers within the industry coalesced to form consortia to take on workforce challenges they had in common.
These consortia infused vibrancy into outdated curriculum, retrained faculty at participating colleges in the latest skill sets, added seat capacity to previously atrophied programs, and stood alongside certificate and degree offerings to signal their intent to hire students. They exchanged tools and practices for their regionalized and localized needs.
Healthcare can rally in a similar way. Solving workforce shortages is better done as a team, not as an individual sport. Additionally, the Governor’s proposed 2023 California state budget offers $1.7B in new healthcare workforce incentive funds that can be more readily tapped when employers collaborate.
As the Nation Grapples with a Mental and Behavioral Health Crisis, Futuro Health Named by California as a State-Approved Provider to Grow Peer Support Specialists
Starting this July, legislation that passed in 2020 will begin changing how the vulnerable in California’s communities receive care. As outlined in Senate Bill 803 (SB 803), the state will now have established requirements for Peer Support Specialist training programs and set competencies for those workers. With the pandemic exacerbating mental and behavioral health issues, a coordinated approach to growing a paraprofessional workforce is a lesson in how to address a pervasive workforce gap.
SB803 recognizes Peer Support Specialists as a reimbursable service and establishes a statewide set of core competencies for training. The bill also opens the service to an additional reimbursement funding stream beyond billing Medicaid. While this has been a key priority for many Californian organizations and multiple versions of this bill were brought forth in the past, the question of who pays for the service had previously held up the progress of the legislation.
Before this legislation, Peer Support Specialists were hired using soft funds or acted as volunteers. Now that PSS services are reimbursable, financial support of these roles has become more concrete. This will mean that more people can and will use these services, explained John Cordova, RN, PHN, BSN, and Director of Workforce Development & Clinical Partnerships with Futuro Health. “We will see these roles expand in more clinics and community-based organizations and even some of the hospitals,” Cordova said.
Peer Support Specialists have lived experience with the process of recovery from mental health or substance use challenges and provide peer support for others experiencing similar issues. While Peer Support Specialists have existed within healthcare for years, SB 803 went a step further by validating the position and bringing the certification process to the state level.
“They’re better able to engage individuals,” said Lucero Robles, the Quality Assurance and Compliance Director for California Mental Health Services Authority (CalMHSA) of peers providing support to people who are in situations the peers themselves have lived through.
“As a social worker, my knowledge of mental health, the medical model, supporting people in the community, that’s what I bring to the table, but a peer brings their recovery, their journey themselves,” she said. “They’re using a lot of themselves in this.”
As Cordova explains, a PSS has the lived experience to tell someone in crisis that they know and understand what they are going through. A counselor can tell a patient to stop using drugs, but a former drug user can speak to their specific life experience. Lived experience is a key component in trauma-informed care for trauma like drug or alcohol abuse, and domestic violence.
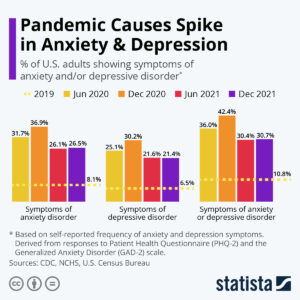
The legislation will be fully implemented starting this summer, which comes at a time when the entire country is feeling the strain of two years of a pandemic, oftentimes at the cost of our mental health.
“The pandemic has been emotionally taxing on every person,” said Robles, who notes that there is and always has been a need for trained paraprofessionals in the field of behavioral health.
As the country also faces a national healthcare worker shortage with employers paying 2-3 times the cost for certain temporary traveler staff, nonprofit Futuro Health has uniquely stepped up to the plate to skill up more trained diverse workers. Futuro Health makes education journeys into allied health career possible by growing the talent that employers need and creating a path to opportunity that workers want. With the implementation of SB803, Futuro Health is going a step further to train Peer Support Specialists as one of the newly announced state-approved providers of this training – set to launched July 1st on the California Services Mental Health Authority website.
Policy and Best Practices Combine to Grow Much Needed Trained Workers
Not only is this legislation an opportunity to address existing healthcare workforce shortages but it is a reflection that peers bring value and experience to the table, said Toby Ewing, Executive Director, California Mental Health Services and Oversight Commission.
Ewing said that while it has been a struggle for years to build an adequate network of services, it has pushed the state to think more creatively about how we define care. Ewing said the legislation shows the state is embracing the perspective that lived experience is important – something the California Mental Health Services and Oversight Commission agrees with and will build upon. Ewing also emphasized that SB 803 ensures certification meets a standardized level of training.
In November 2021, the California Mental Health Services Authority (CalMHSA) and County Mental Health Plans scoped how SB 803 would be implemented. SB 803 established 17 core competencies for Peer Support Specialists. Instead of 58 behavioral health plans for each county, there will now be one standardized process across the state. Experts agree this standardization is key to streamlining the process for training providers. The Department of Health Care Services took the lead in establishing statewide training standards expected from the vendors chosen to provision the curricula.
Futuro Health Incorporates Workforce Best Practices to Ready the Future of Care
Futuro Health, having supported over 5,000 diverse adults tuition-free in pursuing their education for in-demand allied health roles including Medical Assistants, Health IT Specialists, and Patient Care Representatives, was named a state-approved training provider for Peer Support Specialist Certification. Futuro Health’s PSS online offering will include immediate start dates, rapid registration, and off-hour schedules, which will appeal to working adults, Cordova explained.
Futuro Health’s workforce solutions also combine adult-friendly education journeys, live touchpoints, and a scale that meets the state’s expansive geography. Eighty percent of Futuro Health’s students are ethnically diverse, averaging 30 years in age with 51% speaking more than one language.
“The pandemic expanded quality online education and virtual student support options that can be bundled in novel ways to develop interpersonal and technical skills,” said Van Ton-Quinlivan, CEO of Futuro Health. “Futuro Health and our partners combine best practices in workforce development so that employers and states can plug-and-play to accelerate their own endeavors.”
Futuro Health invites education institutions with online and hybrid degree offerings associated with in-demand mental and behavioral health roles to collaborate in building out career paths for upward mobility. Interested education institutions can email partnership@futurohealth.org.
A Playbook for a Post-COVID Workforce: Talking ‘WorkforceRx’ with Experts from Education and Industry
Futuro Health CEO Named Vice Chair of California Health Workforce Education and Training Council 
Sheroes
All month, in honor of National Women’s History month, we have asked our followers to share a story of a woman who has made an impact on their life. Here are just a few of the response amazing responses we received! *